
-
Skin Care Tips for a Radiant Complexion
posted: Aug. 14, 2023.

-
The Power of Chemical Peels
posted: Aug. 01, 2023.

-
Understanding Acne: Causes and Treatment Options
posted: Jul. 13, 2023.

-
Treating Eczema in Adults
posted: Jul. 01, 2023.
-
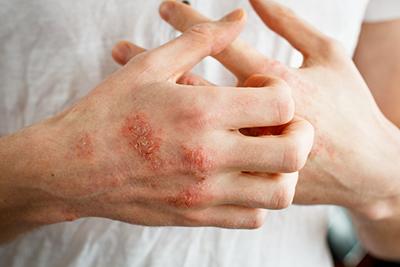
Common Causes of Rashes
posted: Jun. 21, 2023.
-
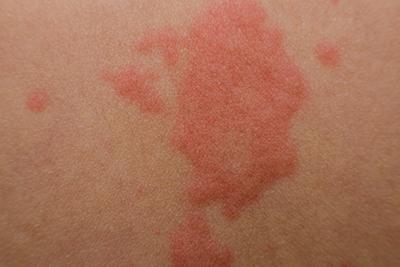
Treatment Options for Acne Scarring
posted: Jun. 06, 2023.
-
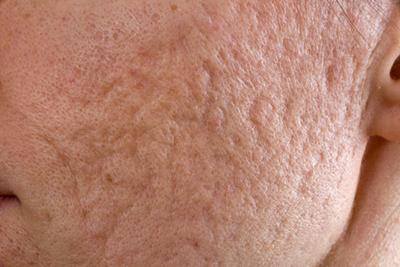
The ABCDEs of Skin Cancer: Understanding the Signs and Symptoms
posted: May 15, 2023.
-
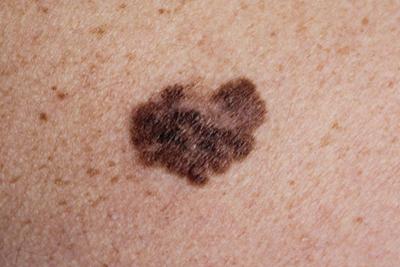
Eczema: Understanding Triggers and Treatment Options
posted: May 08, 2023.
-
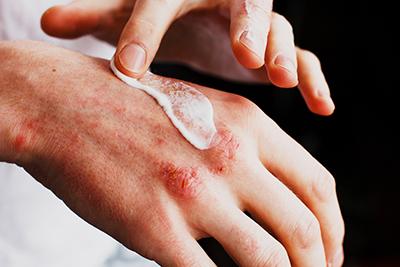
Common Skin Conditions: Eczema, Psoriasis, and Rosacea Explained
posted: Apr. 21, 2023.

-
Skin Cancer Prevention Tips
posted: Apr. 07, 2023.

-
Skincare Tips for Every Skin Type: How to Keep Your Skin Healthy and Radiant
posted: Mar. 23, 2023.

-
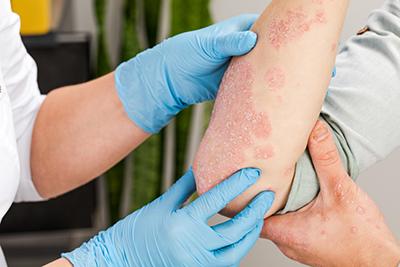
Understanding Common Skin Conditions and How to Manage Them
posted: Mar. 10, 2023.
-
Understanding and Managing Acne
posted: Feb. 27, 2023.

-
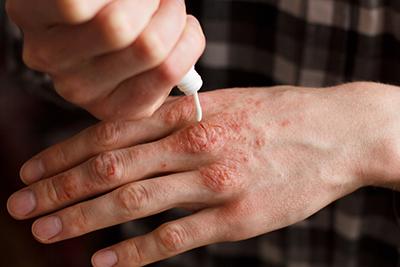
How to Treat and Prevent Eczema Flare-Ups
posted: Feb. 07, 2023.
-
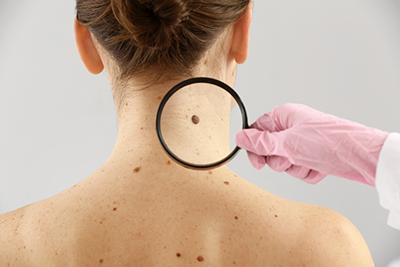
The Benefits of Regular Skin Cancer Screenings
posted: Jan. 24, 2023.
-
Non-Invasive Anti-Aging Treatments
posted: Jan. 11, 2023.
Our Locations
Find us on the map
Shenandoah Dermatology
1600 N Coalter St, Suite 12 & 19
Staunton, VA 24401
45 Commerce Park Drive
Raphine, VA
24472
16 Ivy Ridge Lane, Suite 138
Fishersville, VA 22939
400 S Magnolia Ave Unit B
Waynesboro, VA
22980
3322 Emmaus Road,
Harrisonburg, VA 22801

